News & Blog
We are celebrating a grant of £39,726 from Arts Council England to support our work with older people living with dementia in acute hospital settings!
The funding will support Rhythmix’s Wishing Well Music in Healthcare programme which brings live music making to the bedsides of people living with dementia while they are in hospital.
This new programme will enable our team, of Musicians in Healthcare, to bring their vocal, instrumental and technology skills right to the heart of healthcare. Making music with people at their bedsides helps to shine a light on people’s talents, creativity and life stories; it celebrates what people living with dementia can do and helps support wellbeing during the challenges of hospitalisation.
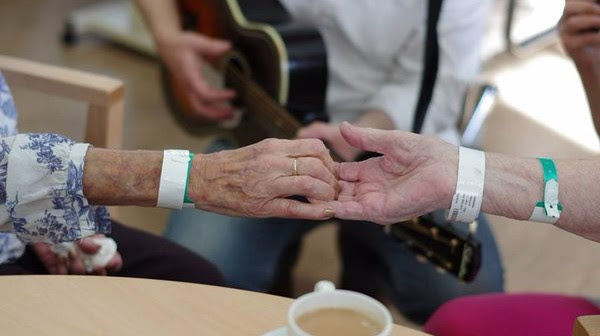
The Wishing Well Musicians in Healthcare are a team, dedicated to bringing creative experiences into hospital settings where music can have a profound impact on wellbeing – get a glimpse of their work in our short films here
Commenting on the grant Jane Humberstone, Vice Chair at Rhythmix, said:
‘’Wishing Well is one of the deepest experiences I have had when observing the impact of music on the brain. Music is part of our everyday life and we all know it is good for us. Many of us are lucky enough to have a life transformed by it. However, to have confirmed that it continues to have such positive effects even into late dementia truly uplifting. I cannot think of a better cause. Thank you to Arts Council England for their continued support for this work.’’
Our team of “Wishing Well” musicians bring music-making right to the bedsides of children and young people in hospital, helping to create positive experiences at a really difficult time for families.

Making music together provides a way of expressing and releasing stress; a moment of fun that has nothing to do with illness or the frightening things that hospitalisation can involve. It’s a very normal thing in fact; playing musical games or singing lullabies with your baby but in the extraordinary world of the hospital, music-making takes on many extra layers of significance.
One of the many challenges for children who are in hospital for long periods of time is that most of the adults they meet are medical professionals who need to carry out uncomfortable, sometimes stressful procedures and interventions. The youngest child will quickly associate “someone is coming into my room” with “something uncomfortable is going to happen” It can put children in a state of stress. Having musicians on hospital wards, as part of the multi-disciplinary team that supports children, can work towards redressing this balance by creating fun, safe, child focused interactions that ask “what can you do?” rather than “what is wrong with you?
One of our Musician’s writes:
“We gently played music by the door to a little boy’s room. A passing Doctor commented “he’ll cry if you go in!” but Mum caught our eye and waved to us. We very gently approached the little boy, crouched down near to him and started singing nursery rhymes, looking for a response to show us which one he liked. He was withdrawn at first, suspicious of what we might do but the introduction of our brightly coloured percussion was too much for him to resist. As he explored the sounds of the different instruments, Mum suggested his favourite lullaby and for a while, we all sat, singing and playing together, all anxiety forgotten and the rest of the hospital, a million miles away.”
The outcomes that Rhythmix work towards and capture have emerged in the course of work in children and young people’s healthcare settings. Our intention to reduce anxiety and isolation and increase self expression is widely supported by the healthcare staff who have helped to shape and guide our work right from the beginning. They recognise both the need to address these issues as part of the care they offer and the effectiveness of live music making in meeting them. In this two part series we explore internal and external factors affecting our work in children’s wards and units and mental health units.

We’ve all felt it. You’re going through your day feeling a bit grumpy, maybe a bit ill or sad, and then a car alarm starts blaring. It get’s into your head. You get irritable, agitated, angry, distressed. We take it out on others, and you go from feeling under the weather to suddenly feeling a whole lot worse.
This is the everyday experience of a child in the pediatric Critical Care unit of a hospital. Dealing with an illness or issue that requires hospitalisation, a child is already feeling anxious, sad and upset. Then they have to contend with beeping machines echoing on plastic floors, the sounds of other people being upset or crying, hurried footsteps and the frequent ominous alarms. The sounds around a person in hospital only make a person feel less at ease on a ward. Coupled with the monitors, wires and apparatus around a hospital bed Critical Care Practitioner Janet Lee of The Alex explains “even our beds don’t look like beds and our tables don’t look like tables. There is little here to make the children feel safe”.
But Rhythmix’s Wishing Well team is making a change to handle both the internal upsets and external factors that make a hospital stay difficult, unpleasant and at times traumatic. By bringing live, interactive music making right to the bedside we are helping improve the experience for children in hospital.
Internal Factors
Amongst the internal factors making a stay unpleasant, babies born in hospital who stay for a long period of time often find it difficult to create attachments to a primary caregiver. This can lead to a lack of resilience and mental health issues in later life. Disabled children spending long periods of their early years in hospital also learn to associate adults with pain and lack of communication due to often being spoken about instead of spoken to. Additionally, family bonds can become strained as there are few opportunities for activities that normalize positive family interaction and activities.
Helping disabled children in hospital develop even very preliminary music skills can help build internal strength. Our Wishing Well musicians help children make music, and families are encouraged to respond with mirroring or complimentary sounds and communication, and encourage and praise any self-expression.
Music making can also be instigated by child or parent as a way of reducing anxiety or loneliness in the long term by providing an ever-present tool that can be used at any time. This allows children to connect to their family in a way that can be carried on at home, or in the hospital when Wishing Well musicians are not there.
A medical student from Brighton and Hove Medical School who observed our work in hospitals in 2016 as part of a placement recognised the rebuilding of internal family bonds thanks to music, explaining “When we go into a room, quite often the family seem disconnected. Parents might be on phones, children are often watching TV but as soon as we start playing music, the family come together. They physically move closer and start to connect more. Parents start to encourage the child and respond to whatever he or she is doing. Laughter breaks out and sometimes tears. The family is drawn together by music”
External Factors
On the external factors, music can distract and ease the pressure from the hospital soundscape and can distract from treatment. Children and young people frequently have medical procedures done to them such as dressing changes or injections. Some of these are uncomfortable, painful and distressing. One staff member commented in the staff survey at The Alex “They played music and engaged with child when I had to do a potentially painful procedure. The child was compliant and it made the child feel relaxed and they were calm throughout making a difficult situation much easier for child and family and staff. “
But what impact is music having in the long term on the young people’s lives? It’s hard to tell. Some of the children we work with have a very uncertain future so the best we can do for them is to have an impact on their wellbeing in the moment of the interaction. We hope that the sense of human connection and calm will stay with them but it is very difficult to collect data that supports an outcome over time with these children. They may experience a sudden change in their health condition that understandably over rides the work we have done with them an hour or two previously. At least some of our work is best evaluated in the moment.
Importantly though, we have an overwhelming amount of evidence from participants, families and staff in feedback, film and surveys that demonstrates just how effective live music making is in reducing anxiety and isolation. When a child has a complicated picture of health, and the future is uncertain, any opportunity to make a period of time better should be relished.
When the external factors such as soundscapes and procedures are distressing, and internally family bonds and communication are weak, music is the tool that can address both of these simultaneously whilst forming happy memories and musical skills.
We are over the moon to announce that Programme Director, Jo White was announced winner of the Musician’s Union “Inspiration” Award 2018 for her work with the Rhythmix, Wishing Well programme! In just 4 years Wishing Well has grown from a pilot project at The Royal Alexandra Children’s Hospital in Brighton, to a Sussex wide Music in Healthcare programme working in partnership with 6 NHS Trusts. Every week, our Musicians bring music making into hospitals across Sussex and Surrey to work as part of the hospital team, helping to improve people’s stay in hospitals and reduce some of the anxiety that people can feel. We receive such incredible feedback from the families that we work with about how music making has helped their child or an older relative through a difficult time; music really can reach places that medecine can’t and we are looking forward to many more years of making music where it is really needed.

Programme Director Jo White is taking a 24 hour sponsored challenge for Wishing Well!
“The music starts…and it all comes flooding back”
We urgently need to raise funds so that we can keep bringing the extraordinary benefits of music making to people who are living with dementia.
So – I am organising a fund-raising, music-making, non-stop 24-hour jam in Brighton. I will play music for 24 hours pretty much non stop using my voice, my accordion, music technology, percussion and anything else I can think of from sunrise on the 25th until sunrise on the 26th November. I will be joined throughout the 24 hours by a whole load of musicians friends; community choirs, fiddle players, sing songwriters, experimentalists and improvisors. The event will take place in the exquisite Regency Ballroom of Angel House, right on the seafront in Brighton. I’m, slightly nervous…and very busy pulling together creative ideas and sorting logistics but I am very very excited!
I want to fundraise personally and creatively for people with dementia because every single day in our work we see the difference that music makes. The late great Oliver Sacks called music ” the past embedded in amber”. I think of it like this; when we make music with people that is meaningful to them, it’s like shining a light on who they are; personalities shine through and they are illuminated. They connect outwards again “like a flower unfurling”
Please help us support people with dementia
You can sponsor me through my JustGiving page here
Or TEXT WWJO48 £5/£10/£25 to 70070

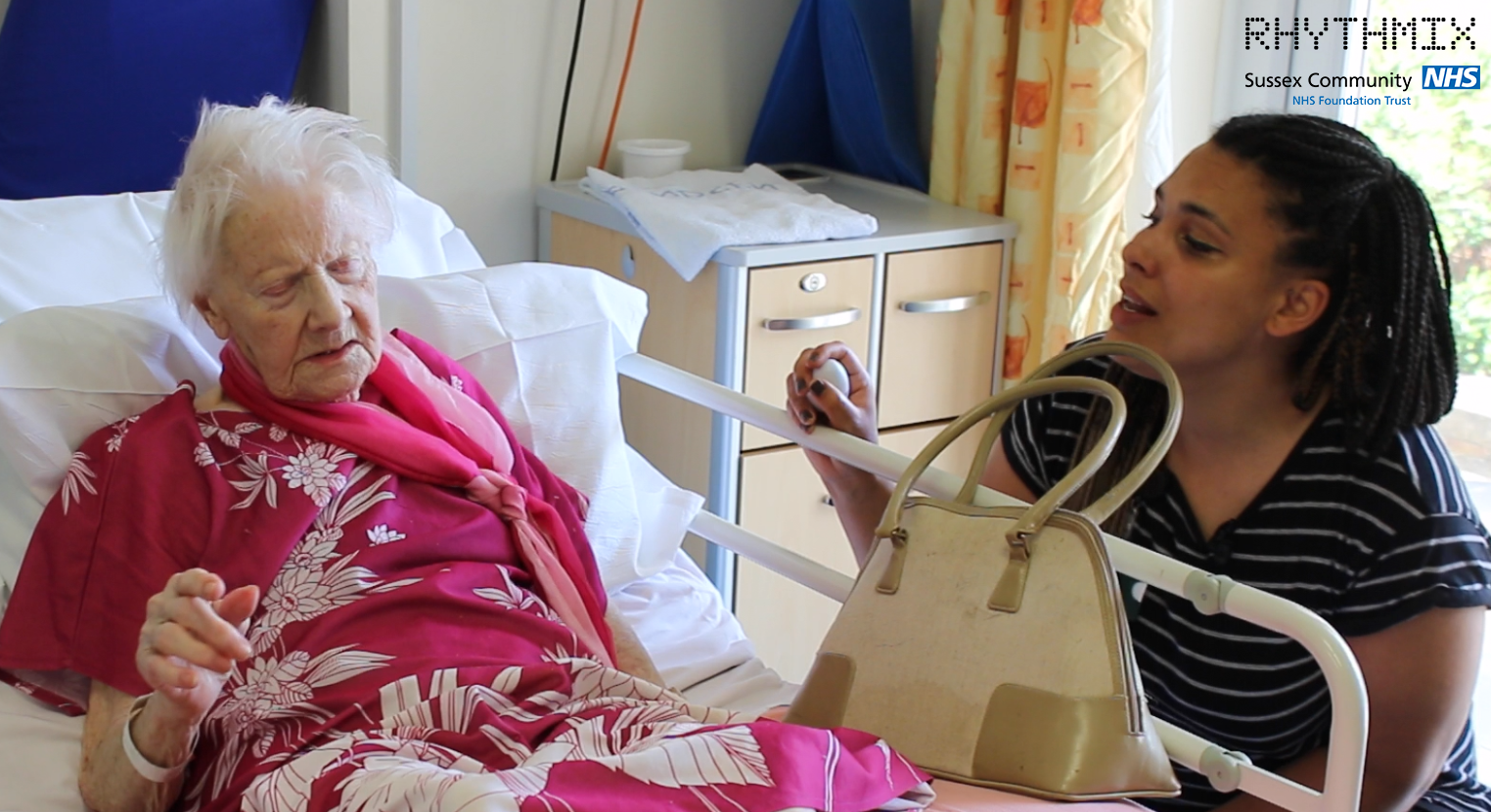
We’ve been working with people with dementia at Arundel Community Hospital in West Sussex as part of a research study with Sussex Community NHS Trust. A few of the many beautiful moments of joy and connection shared between musicians, patients, families and nursing staff are captured here in this short film commissioned by Sussex Community Foundation NHS Trust and made by West Creative.
The study investigates how live music making helps people with dementia and their families feel less anxious and better connected during their hospital stay. Are musicians a valuable resource for busy hospital wards? Does making music help hospital staff to engage in meaningful ways with their patients? We’ll be sharing the findings later this year.
You can watch the film here